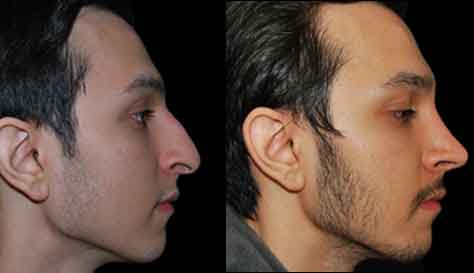
Facial Paralysis Surgery
Conveniently located to serve the areas of New Jersey and New York

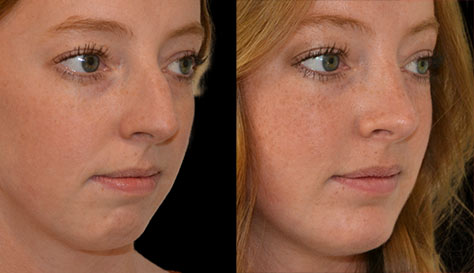
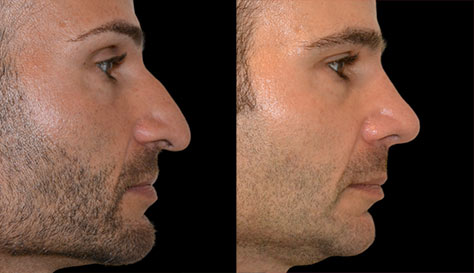
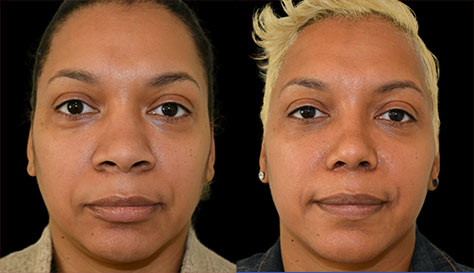
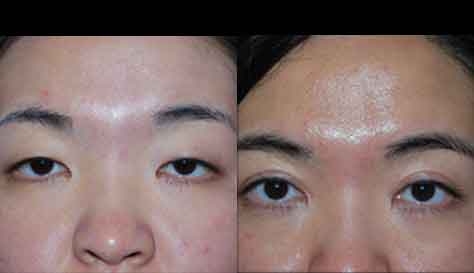
Facial paralysis is a condition where one or both sides of the face are either very weak or completely immobile due to the malfunction of the facial nerve. Not surprisingly that this condition causes not only multiple functional problems, but also carries with it a tremendous psychological impact. Individuals with facial paralysis are unable to fully close the eye (on the paralyzed side) which can lead to the dryness of the cornea with loss of vision and even blindness, suffer from excessive tearing due to lower eyelid weakness, have difficulty eating and speech problems due to lip weakness, and suffer from facial asymmetry and disfigurement.
There have been described over 80 potential causes of facial paralysis, however Bell’s palsy, trauma, infections and neoplasms account for almost 80% of the cases.
Given a significant functional and psychological burden on the patients, it is very important to be able to help individuals with this condition improve their appearance and regain lost functions.
Theoretically, the ideal facial reanimation should try to achieve: facial symmetry at rest, symmetry with voluntary and involuntary motions, and restoration of the functions of the eye, nose, and mouth without compromising function and appearance of other areas of the face.
There are multiple surgical and non-surgical procedures available to help patient with facial paralysis. Among non-surgical modalities, neuromodulator treatments and physical therapy are the most commonly used ones. neuromodulator treatment helps to improve facial symmetry; it also helps with facial ticks and abnormal facial movements (synkenisis) by relaxing certain muscles causing the problem.
Surgery remains the mainstay treatment for long-standing facial paralysis. Some surgical procedures are aimed at restoring facial movements and function by either using patients own non-paralyzed muscles (such as temporalis muscle), bringing muscles and nerves from other areas of the body in the form of a free flap, or restoring the integrity of the facial nerve itself (if possible). In addition, there are many adjunctive surgical procedures to help the eye, such as gold or platinum upper eyelid weight insertion to improve eye closure as well as tightening of the lower lid to improve its support and reduce tearing. Other adjunctive procedures help correct brow ptosis (browlift), facial laxity (facelift), and facial asymmetry (facial slings).Dr. Ovchinsky has many years of experience of successfully helping the patients with facial paralysis to regain their lost identity and function. If you are suffering from this debilitating condition and in need of assistance, please call Plastic Surgery of Short Hills to arrange for in-depth consultation.
FAQ
What do I need to avoid before surgery?
If you are on “blood thinners,” you will be asked to stop them approximately one week prior to surgery. We also ask that you avoid certain over-the-counter medications. If you are taking some herbal supplements, you should stop those as well as they may contain blood thinning substances. Also, you have to completely quit smoking at least two weeks before surgery.
What about my daily medications before surgery?
You will have a preoperative appointment well in advance of your surgery when we will review all mediations with you. If you are on “blood thinners,” you will be asked to stop them approximately one week prior to surgery. We also ask that you avoid certain over-the-counter medications. You may continue taking most routine medications up until the morning of surgery with a small sip of water.
What happens after surgery?
You will go to the recovery room for a few hours until you are fully recovered from anesthesia. Once you are stable you will be taken home (or to a hotel) by your family member or a friend. You will want to stay relaxed for the first few days. You will need to keep your head elevated when in bed to help with faster resolution of swelling. You should begin to start walking, eating, and using the restroom the day after surgery. Your activity can slowly increase each day but it will take up to 2 weeks before you start to feel like your old self again. You should avoid any strenuous activity for 4 weeks. You will need to take medication prescribed to you by Dr. Ovchinsky, which usually include antibiotics, pain medicine, antibiotic ointment for the incisions, and occasionally anti-nausea medications.
Are there any dietary restrictions following surgery?
No. Patients can eat whatever they want. Advance your diet from liquids (fruit juice, milk shake, etc.) to soft food (pudding, macaroni and cheese, mashed potatoes and gravy, oatmeal, pasta) to solids as tolerated. To prevent dehydration, please drink as much juices and nutritional fluid as possible.
When will my stitches be taken out?
Stitches are normally removed five to six days after your surgery.
How soon will I be able to exercise?
Dr. Ovchinsky recommends that patients do not return to exercise for three weeks after their procedure.
When will I be able to see the results?
You may see the difference right away, and more so once the swelling goes down within the first one to two weeks. As with any surgical procedure, it takes anywhere from 6 to 12 months for the results to become final.
What is special about the way Dr. Ovchinsky does the surgery?
Dr. Ovchinsky tailors his surgical technique to an individual patient rather than using the same “run of the mill” surgery on everybody. The technique he uses causes minimal pain, has natural results, and is long-lasting. The vast majority of patients are quite surprised afterward at how little discomfort they have and how quickly they return to normal activity. Most patients have minimal bruising. Finally, with Dr. Ovchinsky technique and attention to details during skin closure, scars are typically minimal and are often difficult to see once they have fully matured.